Doctors deal with death all the time. But they still struggle to tell a patient they’re dying or help them live with a terminal disease. A specialty called Palliative Care is trying to change that. It’s been around since the 1990s. But a lot of people, even in the medical profession, still don’t know it exists.
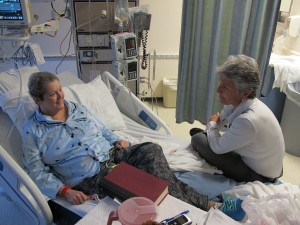
Dr. Linda Smith walks into a room at Providence hospital ready with a stethoscope and a huge grin. She teases that Dawn Dillard’s spiky hair recently resembled a faux hawk.
Dillard found out she had uterine cancer a year ago, on her birthday. By the time she got the diagnosis, the cancer had spread to her liver and lymph nodes. Her oncologist gave her a year to live. The 57 year old beat those odds. But now her kidneys are failing. After the laughs are over, Smith sits down on the edge of Dillard’s bed, leans in, and starts talking about a procedure Dillard will have.
Smith is a palliative care doctor, a specialty that is growing rapidly in the U.S. The idea is to help patients cope with a terminal or life altering illness. And unlike hospice care, it is not offered only in the final months of life. Smith works on pain management, coordinating care and even does some counseling. Her goal is to improve her patients’ quality of life. She calls it “whole person care.” Dillard thinks that’s accurate:
“I can’t even say how much she’s helped me. Just little things. You know, showing me things like breathing techniques. Sort of like mediation, just ways to focus on things that are positive and happy rather than focusing on your sickness and how crappy you feel.”
Two years ago, Linda Smith was a very different kind of doctor. She worked in the Emergency Room, where the goal was to quickly stabilize a patient and move on. But two decades into her career, she started to question how she was caring for patients at the very end of their lives. She remembers putting patients on breathing tubes, and hearing family members say things like, ‘I know dad didn’t want this, but we’re just not ready to let him go.’
“I started to have a lot of regret about doing things to people that were painful and uncomfortable and were prolonging their suffering. And if I only had the time to sit down with the family, I probably wouldn’t be doing these things.”
Reporter: And did you know about palliative care?
Smith: “I’m laughing. The answer is no. I didn’t know. And in fact when I started looking into palliative care, I got online… and low and behold I saw that we had a palliative program here at the hospital I was working at.”
In the summer of 2011, Smith enrolled in a one year palliative care fellowship at Providence. It wasn’t easy at first. She wanted to roll up her sleeves and start helping right away. Her mentor, Dr. Steven Rust wanted her to wait. He remembers it this way:
“When she started, she would literally say to me, and she’s the only person that calls me this, she’d say, Boss? Put me in the game. And gently I hope, I just said, ‘let’s wait a little bit longer.'”
Smith had a lot to learn. She was a bad listener. And she was busy. As an ER doctor, sometimes she didn’t even sit down to deliver devastating news:
“I can remember saying to families things like, ‘I’m sorry there’s nothing more I can do.’ And I realize now that sounds like abandonment to many people when you say you can’t do anything more. And the reality is I may not be able to do anything more to the patient that will make them survive, but there’s a lot more that I can do. I always can do more.”
A lot of what Smith does is talk to people. She doesn’t advocate for or against treatment, but she wants patients and their families to understand their decisions. If a doctor puts in a breathing tube, for example, that may extend a patient’s life, but they won’t be able to eat or talk. If they die with a tube in, the family will miss hearing their last words. So now Smith sits down for hard conversations and looks patients and their family members right in the eye. Earlier this year, she was called in to consult with the wife of a patient who was dying:
“When I entered the room, the wife said to me, ‘I know who you are.’ And I said, ‘oh. ok’And she said, ‘I don’t want to talk with you and I don’t want to like you because you’re here to talk about death and dying aren’t you?’”
Smith had a short conversation with the woman, and left her a book on difficult end of life choices. She went back to visit her the next day:
“And she said, ‘you know, I so tried not to like you. And what you had to say. And I really realize that we need to have this discussion now, don’t we?’ And I said, ‘when you’re ready, we’re ready to have that discussion.’ and she said, ‘I’m ready now.’”
Smith was planning to return to the Emergency Room. But interactions like that one persuaded her to stay in palliative care. Now she works more and makes less money. Some days, she wonders if she’s crazy. But then she gets to visit a patient like Dawn Dillard. Back in her hospital room, Dillard asks Smith if she really needs to have yet another procedure.
Smith gives Dillard a hug and plants herself at an empty desk at the nurses’ station outside her room. She calls Dillard’s other doctors and realizes the second procedure isn’t really necessary after all. So instead of staying another night in the hospital, Dillard and her husband are back home by the end of the day.
This story is part of a reporting partnership that includes APRN, NPR and Kaiser Health News.
Annie Feidt is the broadcast managing editor at Alaska Public Media. Reach her at afeidt@alaskapublic.org. Read more about Annie here.





