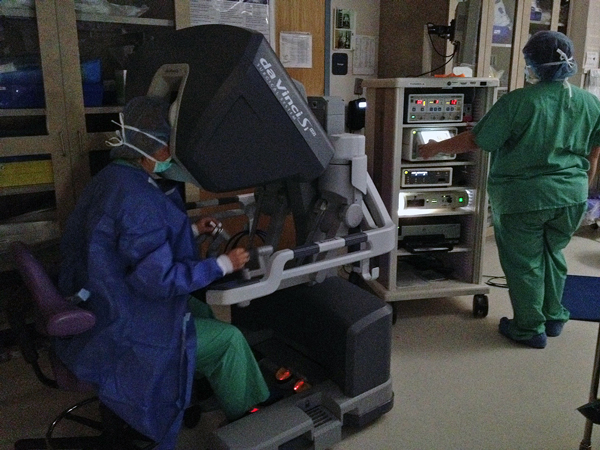
Surgeons these days have a lot of futuristic tools at their disposal in the operating room. They use robots, high definition cameras and special dyes to help them complete complicated procedures. And you don’t have to travel to big cities in the Lower 48 to find the most up to date operating room technology.
Miranda Studstill is 24 years old. And for the past two years, she’s been in near constant pain.
“It’s just like a searing, stabbing pain. It feels like… your insides are like play dough and somebody’s digging their fingernails into it. It hurts so bad.”
Miranda has endometriosis, a disorder where tissue that usually lines the inside of the uterus, grows outside of it instead. And lately, her life has been dictated by the disease. She’s endured three surgeries so far. When I meet her for the first time in a doctor’s office in East Anchorage, she’s preparing for surgery number four.
Her surgeon, Dr. Donna Chester lays out the plan for the next morning. She is going to remove Miranda’s right ovary and any endometriosis she sees. She’s hoping that will relieve her pain.
Less than 24 hours later, Miranda is under anesthesia on an operating table at Alaska Regional. It’s hard to even see her under a mound of sterile blue drapes. And Dr. Chester is not standing over her. She’s ten feet away- sitting at a console that looks like a high tech video game.
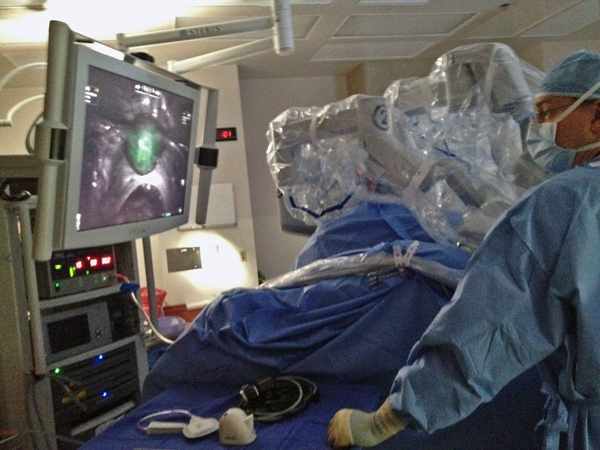
The robot is called a da Vinci. Chester’s hands are on two controls that manipulate robotic instruments inside Studstill. TV screens illuminate what the cameras attached to those instruments are capturing. As Chester moves the controls, the instruments respond, snipping tissue apart that is stuck together. They’re called adhesions, and they can be very painful for patients like Miranda.
Chester doesn’t see much else near the right ovary that is a cause for concern. She pops up from the console:
“Since all that pain was because of that adhesion, I can leave that ovary in, I mean, she’s only 23 I hate to take an ovary out.”
To make sure she’s not missing anything, Dr. Chester uses a new technology called Firefly. It’s a bright green chemical dye that will light up any endometriosis Chester can’t see with the robotic cameras.
“It’s a dye that goes in there, and any area that has endometriosis is more hypervascular and it’s supposed to show it up more. I’m not seeing any additional stuff in here. Which is good for her- all she had were the adhesions. And… that’s so much better.”
Chester goes out to the waiting room to check in with Miranda’s mom, and then comes back to close up the four small incisions. She does that the old fashioned way- without a robot. She’s pleased with how the surgery went.
“I think she’ll feel the pain difference almost immediately when she wakes up.”
As for Miranda, she was thrilled to be able to keep her right ovary:
“When I woke up in the recovery room, that’s the first thing my mom said, ‘you still have it’ and I started crying, it was really, really awesome.”
I meet with Miranda less than two weeks after the surgery. She has already started back at her job as a court reporter. And her pain is a lot better:
“It’s still kind of there but it’s so much better, it’s not the first thing on my mind now.”
She says she’s eager to get her life back:
“I’m really hoping that it will change everything. The last two years my life has really been on hold because I’ve been so sick and it’s been so difficult.”
Miranda’s hoping this is the last surgery she’ll have to go through for a long while.
Annie Feidt is the broadcast managing editor at Alaska Public Media. Reach her at afeidt@alaskapublic.org. Read more about Annie here.





